Introduction
Milialar, often known as “milk spots,” are uncommon skin blemishes that may frighten some people. It’s crucial to comprehend the causes, signs, and possible treatments for these benign, small cysts. This comprehensive manual aims to provide insights into the world of Milialar, valuable for anyone attempting to address or avoid them.
Contents
What is Milialar?
Familial Hypercholesterolemia (FH), another name for Milialar Disease, is a hereditary condition that impairs the body’s capacity to eliminate LDL cholesterol from the blood. Although cholesterol serves a vital function in our systems, when levels become excessive, they can lead to serious health problems like heart disease and stroke.
Milialar disease patients have a unique gene mutation that hinders the liver from properly avoiding low-density lipoprotein (LDL) cholesterol, which is typically referred to as “bad” cholesterol. LDL accumulates in the bloodstream and in the artery walls as a result, which causes plaque to develop.
Reasons for Miliarlar
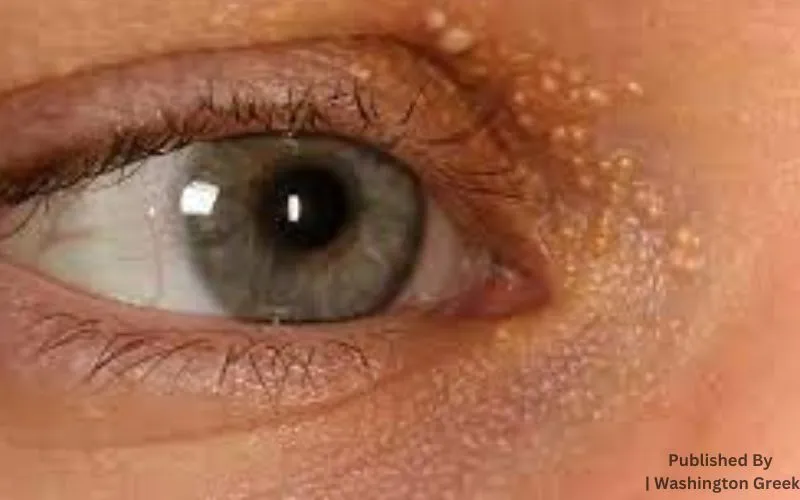
Milialar are tiny, brittle cysts that develop beneath the skin. Keratin, a protein present in skin, hair, and nails, is present in them. Milialar often takes the form of tiny white bumps on the face, particularly near the eyes, nose, and cheeks.
There are a few common causes of Milialar:
- Genetics: Milialar is genetically based and typically runs in families. You are more likely to get milia if either of your parents did.
- Harsh skin care products: Strong chemical cleansers, toners, and exfoliants can damage the skin’s barrier defenses and strip the skin. Milia are more prone to develop as a result. Use moisturizing skin care products that are mild and tailored to your skin type.
- Dry skin: Dead skin cells have a tougher time sloughing off dry skin. As a result, keratin and dead skin cells may become stuck and develop Milialar. This can be avoided by using a heavy moisturizer, especially around the eyes.
- Certain medications: Milialar can develop as a side effect of certain drugs, such as steroid creams. If you suspect that a medicine may be the source of Miliaryar, consult your doctor. Frequently, modifying or switching the medicine can aid in Milialar resolution.
- Sun exposure: Milialar risk is heightened by excessive keratin production brought on by UV damage to the skin. To protect your skin, use a daily broad-spectrum sunscreen.
The good news is that while they might be bothersome, milia are normally harmless. Professional extraction performed by a dermatologist or esthetician is the most successful treatment. Maintaining proper skin care and hydration at home can also help maintain your skin clear and healthy and stop the development of new milia.
Symptoms of Milialar
Milia, which are small cysts that develop just below the skin’s surface, is one of this condition’s symptoms. The extra keratin protein found in hair, nails, and the outermost layers of dead skin cells accumulates beneath layers of dead cells and becomes trapped beneath these dead layers, causing tiny little lumps, known as milia, to form. Typically, they show as clusters of painless pearly white or yellowish protrusions on either the face, such as the nose or cheek areas, or the trunk or genitalia.
Milialar rarely hurts, although it could itch if it becomes infected or inflamed. It is best to consult a dermatologist for a proper diagnosis and therapy of these spots because they could also be symptoms of more serious underlying conditions.
Milialar lesions typically have small raised bumps or lesions that are painless and dome-shaped on the skin, such as eyelids, lips, cheeks, or beneath your eyes. Milialar lesions are typically simple to identify on your own. Milia can appear everywhere on the body, but older people and babies seem to notice them more frequently on their faces than anywhere else.
Older persons are known to experience plaques of milia more frequently, which are characterized by numerous, overlapping cysts that produce an opaque or translucent region of skin. Despite being rare, this type of military may develop near the mouth, nose, and eyes, among other places on the body.
Other signs of milia include excessive oil production that clogs pores and traps dead skin cells, as well as hormonal changes associated with puberty, pregnancy, or menopause that influence sebaceous gland size and cause thicker, drier skin that is more likely to catch these particles. Some people find respite from the military by exfoliating frequently and using moisturizers, while others find relief from pharmaceutical creams or laser procedures.
Diagnosis for Milialar
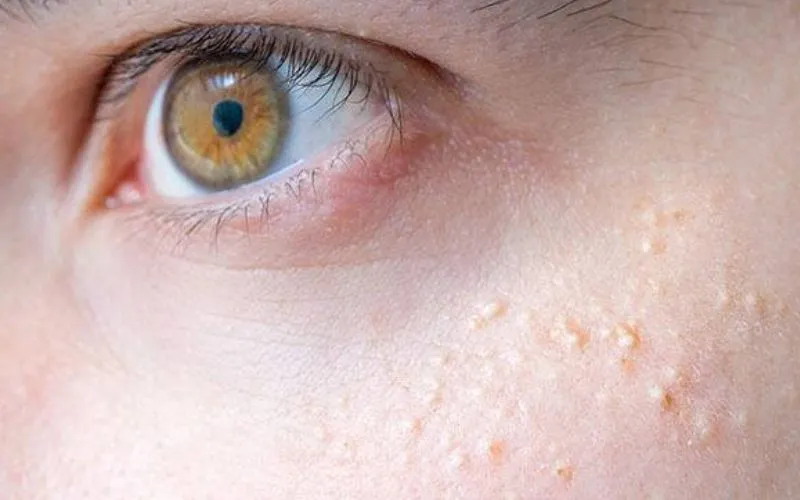
The first step to good treatment is acknowledging the military. The appearance of these cysts on your skin typically triggers a visit to your dermatologist, and because to their distinctive characteristics, they are simple to identify by trained eyes. To make a definite diagnosis, a skin biopsy may occasionally be needed.
There are several treatments available to get rid of military cysts swiftly and without pain or delay after a diagnosis. One such painless method is topical retinoids, which may hasten the skin’s natural exfoliation processes and diminish the size of the milia over time. Other patients choose cryotherapy, which includes freezing milia with an external device for quick relief without pain.
Surgery is another cutting-edge treatment for military ailments. Incision and drainage, a method frequently used by dermatologists, entails making a small incision and draining the area’s contents through it. It can be beneficial but may cause scars. Another efficient method of removing lesions without the need for sutures is a laser technique, in which the lesions are targeted by blasting beams of light at them instead.
Milialar illness may affect a number of body organs or systems, and its symptoms can range from lung problems like shortness of breath or coughing to eye problems like blurred vision and light sensitivity. Milialar users are more likely to experience these side effects.
Genetic alterations may contribute to the development of milialar, although researchers are yet unsure of its exact cause. Skin cells that have undergone mutations may produce excessive amounts of oil, clogging pores with dead skin. Increased oil production brought on by hormonal changes during adolescence, pregnancy, and menopause as well as thicker skin that is more likely to trap dead skin cells may also contribute to blocked pores.
Types of Milialar
Milialar comes in a variety of forms and can show up on different parts of the body and face. The primary and secondary milia are the two most prevalent types.
Primary Milialar
Primary Milialar, often referred to as Milialar en plaque, develops when skin cells are entrapped beneath the skin’s surface. This is most frequent in newborns and frequently goes away after a few weeks. Primary milia in adults are typically located on the forehead, cheeks, and eyes. Primary milia develop due in part to genetics. For aesthetic reasons, the trapped keratin cysts can be eliminated through extraction or laser therapy.
Secondary Milialar
Skin injury leads to secondary malignancies. They develop when damaged skin heals from burns, dermabrasion, or skin grafts. The Milialar is created when new skin grows around trapped keratin. Secondary Milialar can also result from steroid creams or ointments used to treat skin disorders including eczema or psoriasis. Secondary Milialar cannot go away until the original disease or skin injury has healed. Any residual cysts can be treated with laser therapy or extracted.
Milialar brought on by specific drugs or skin conditions is one of the less frequent forms of Milialar. Milia en plaque, or clustered milia, may need to be treated with oral medicine or light therapy. A skin disorder like basal cell nevus syndrome that is inherited can also show up as several Milialar in one place. Consult a dermatologist for a precise diagnosis and guidance on the best course of action to get rid of your Milialar.
Most Milialar forms are treatable with the right diagnosis and care, resulting in clear, healthy skin. The best method to identify the origin of your milia and develop an effective treatment strategy is to speak with a board-certified dermatologist.
Milialar: A Type of Milialar Around the Eyes
Milialar that develop around the eyes, usually on the eyelids, are referred to as milialar. Milia, which are tiny, hard cysts, develop when keratin becomes trapped under the skin. The creation of little white lumps is caused by the keratin’s inability to shed.
The most common causes of Milialar include:
- Genetics: Milia can happen to some people more easily than others, especially around the eyes. Milialar is frequently inherited and runs in families
- Aging skin: Age-related decreases in collagen and elastin production make it more challenging for dead skin cells to shed. As a result, keratin may end up trapped under the skin and result in milia.
- Dry skin: Dead skin cells can become trapped beneath the skin when the skin is extremely dry, which can cause milia to form. The use of moisturizers, particularly those with hyaluronic acid or glycerin, can enhance skin moisture and help prevent acne.
Treatment of Milialar
Extraction is the most efficient Milialar treatment, in which a dermatologist breaks apart the cyst and removes the keratin that has become stuck inside. A sterile needle or blade is used to open the cyst during the treatment, and then the contents are gently pushed out.
To stop milia from forming, topical retinoids or vitamin A creams may also aid in improving cell turnover and loosening keratin in the pores. Retinoids should be used with caution since they can irritate the sensitive skin around the eyes.
Keep skin properly moisturized, use broad-spectrum sunscreen every day, and stay away from harsh skin care products to stop milialar from recurring. Hyaluronic acid, glycerin, niacinamide, or retinol may maintain skin supple and encourage cell turnover in an eye cream.
Milialar is usually not harmful, but the white lumps might be unsightly. For assistance with professional extraction and advice on ongoing prevention and treatment, consult a dermatologist. milialar can frequently be well controlled with routine treatment and observation.
Treating Milialar: Prevention Tips and Removal Options
Prevention Tips
Dermatologists advise the following measures to help prevent milialar from recurring:
- To protect your skin from UV damage, use a broad-spectrum sunscreen every day. The most common cause of milialar is excessive sun exposure.
- Use a face scrub, a chemical exfoliant like glycolic acid, or a facial brush like a Clarisonic to routinely exfoliate your skin. Dead skin cells might obstruct hair follicles if they aren’t removed.
- Use an over-the-counter topical cream with retinoids, which are vitamin A compounds that have been demonstrated to increase cell turnover and maintain clear pores.
- To get blackheads or whiteheads professionally removed, visit a dermatologist. The risk of milialar can rise if these are left in place.
- To keep your skin hydrated, moisturize every day. milialar outbreaks are more likely to occur on dry skin. Choose a non-comedogenic moisturizer to avoid pore clogging.
- Benzoyl peroxide, salicylic acid, and lactic acid are three over-the-counter drugs that are beneficial in reducing the appearance of milia.
- Oral Antibiotics: If the illness is severe enough, a doctor may advise taking an oral antibiotic such as doxycycline or amoxicillin.
Removal Options
The most common removal techniques for milialar include:
- Extraction: A dermatologist removes the milialar cysts using sterile tools. Although it has a high rate of success, this procedure could leave scars.
- Laser therapy: A dermatologist can remove the milialar cysts by using focused light pulses. Although it can be expensive and requires numerous treatments in order to be effective, this procedure normally leaves little scars.
- Prescription creams: In order to dry out and get rid of milialar cysts, a dermatologist may recommend retinoid treatments like Retin-A. This technique has a low chance of leaving scars but calls for diligent application over weeks or months.
- Minor surgery: A dermatologist might need to do minor surgery to remove the cysts if the milialar is severe or chronic. Although it has the largest chance of leaving scars, this approach is quite effective.
Clinical Trials for Milialar Disease
Clinical trials are essential to furthering medical knowledge and enhancing patient outcomes as researchers work to develop more effective therapies and potential solutions for Milialar Disease. Patients get the chance to participate in these trials and gain access to cutting-edge treatments that are not currently on the market.
By evaluating novel medications or therapeutic modalities, trial participants have the opportunity to directly advance science. Scientists can better grasp the effectiveness and safety of experimental therapies for Milialar Disease thanks to the information gathered from these trials.
Individuals with Milialar Disease may benefit in specific ways by taking part in clinical trials. They are closely observed and cared for by a group of medical professionals with expertise in their disease. They are given access to perhaps ground-breaking treatments that could have a big influence on their quality of life.
It’s crucial to remember that joining a clinical trial is completely voluntary, and people should think carefully about the advantages and disadvantages of doing so. Each study also has unique eligibility requirements that must be met.
Consult your doctor or seek advice from research organizations that focus on rare diseases like Milialar if you’re interested in learning more about Milialar Disease clinical trial alternatives. They can guide you through the options that are available and give you useful details about current studies.
Keep in mind that clinical trials are more than simply tests; they stand for the possibility of better therapies and, eventually, a cure for Milialar Disease!
Frequently Asked Questions
What is Milialar Disease, and how does it affect cholesterol levels in the body?
Milialar Disease, also known as Familial Hypercholesterolemia, is a genetic condition that impairs the body’s ability to remove LDL cholesterol from the blood. This leads to elevated LDL cholesterol levels, increasing the risk of heart disease and stroke.
What are the common causes of Milialar or Milia?
Milia, the small white cysts that form under the skin, can be caused by genetics, dry skin, harsh skincare products, sun exposure, and certain medications.
What are the typical symptoms of Milialar?
The main symptom of Milialar is the formation of tiny cysts known as milia just beneath the skin’s surface. These appear as small, painless, pearly white or yellowish bumps, often on the face.
How is Milialar diagnosed?
Milialar is typically diagnosed through visual examination by a dermatologist. In some cases, a skin biopsy might be required for a definitive diagnosis.
Are there different types of Milialar, and if so, how do they differ?
Yes, Milialar comes in various types, with primary and secondary Milia being the most common. Primary Milia form when skin cells become trapped, while secondary Milia result from skin damage or trauma.
What are the treatment options for Milialar?
Treatment options for Milialar include extraction, laser therapy, prescription creams, and minor surgery. Prevention measures like sunscreen use, exfoliation, and moisturizing are also important.
Are there any clinical trials or research efforts focused on Milialar Disease?
Yes, clinical trials play a crucial role in advancing research on Milialar Disease. They offer potential benefits for patients by testing innovative therapies and contributing to scientific progress. Individuals interested in clinical trials can seek guidance from healthcare providers or research organizations specializing in rare diseases.
Conclusion
In conclusion, Milialar Disease, also known as Familial Hypercholesterolemia, is a genetic condition that significantly impacts the body’s ability to regulate cholesterol levels, specifically the removal of LDL cholesterol from the bloodstream. This disorder poses a serious health risk as it can lead to elevated cholesterol levels, increasing the likelihood of heart disease and stroke. While the article delves into the causes, symptoms, diagnosis, and treatment options for Milialar and its associated skin condition Milialar, it is important to emphasize that early detection, proper management, and preventive measures play a pivotal role in mitigating its health consequences.
Furthermore, the article highlights the promising role of clinical trials in advancing our understanding of Milialar Disease and improving treatment options. Clinical trials not only offer hope for those affected but also contribute invaluable data to the scientific community. As ongoing research efforts continue to unravel the complexities of this genetic disorder, individuals with Milialar Disease, their families, and healthcare providers can look forward to more effective therapies and, ultimately, the prospect of finding a cure. In the quest for improved outcomes and a future free from the burdens of Milialar Disease, collaboration between patients, researchers, and healthcare professionals remains paramount.
You can also read about: